Breast Cancer – some lessons
While researching this topic I came across some really interesting facts that some of the Medical Industry seems to be taking notice of. However, because of these facts not a lot of Oncologists are taking any action – they work on getting as much money as possible into their bank account, so why would they use Cancer Killing products or methods that do not provide kick backs from the Manufacturer.
Anyway, first things first.
Breast cancer is not what most people think.
Why conventional therapies fail to turn the tide against the second highest cause of death in the Western world.
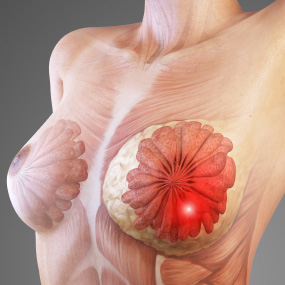
A new study published in The Journal of Steroid Biochemistry and Molecular Biology showed that Vitamin D targets the most malignant cell type found within breast cancer, the cancer stem cells, and is much better than radiation and chemotherapy in targeting these cells. Also vitamin D does not have the damaging side effects of conventional cancer treatment.
Vitamin D, of course, is designed to be manufactured through the ultraviolet B-stimulated conversion of the cholesterol metabolite 7-dehydrocholesterol in the human skin. The fact that in this modern age the breasts are never (or rarely) exposed to sunlight and that generally speaking adequate sunlight exposure (especially considering the over-use of vitamin-D blocking and carcinogenic petroleum-based sunscreens) is rare, it is likely that many of the variations in internal breast structures that are increasingly being diagnosed through technologies like mammography as being ‘abnormal’ or ‘precancerous,’ directly reflect a deficiency of sunlight and Vitamin D.
And since vitamin D3 supplementation is affordable and extremely safe relative to commonly prescribed pharmaceuticals like Tamoxifen (a known carcinogen), it may provide those at risk for breast cancer or breast cancer recurrence with a reasonable alternative to watchful waiting and/or preventive chemotherapy.
This new study identifies an overlooked root cause of breast cancer (cancer stem cells), as well as the use of sunlight exposure (or Vitamin D supplements) as a natural intervention that has yet to be incorporated into the conventional standard of cancer care. There is no money in it for Oncologists, so it is rarely offered as an alternative treatment.
It is actually the existence of the much smaller number of cancer stem cells which causes cancer recurrence, as they are not only resistant to conventional chemotherapy and radiation, but their numbers can actually be increased (enriched) by these two ‘therapies.’ Therefore, any cancer therapy that ignores the cancer stem cell sub-population in favour of killing the normal daughter cells in order to shrink the tumor, will not result in destroying the root of the cancer (the cancer stem cells). In fact, it can generate the illusion of ‘remission’ while in fact making the remaining tumour colony far more malignant, setting up the conditions for aggressive recurrence years later.
The new study focused on a type of breast tissue abnormality known as ductal carcinoma in situ (DCIS), which for decades was considered cancer (constituting about 20% of all breast cancer diagnoses), but recently has been identified as a benign lesion of epithelial origin. There are cases where DCIS progresses towards another breast abnormality known as invasive ductal carcinoma (IDC), which is considered a more serious risk. But even IDC cases may never progress to cause symptoms, nor ever cause harm to those within which it occurs. Nonetheless, the conventional medical system still considers a diagnosis of either DCIS or IDC justification for aggressive interventions, e.g. lumpectomy, mastectomy, radiotherapy and chemotherapy, indicating that if there is a natural intervention to slow the transistion from DCIS to IDC, especially if it focuses on targeting and/or reducing the growth of breast cancer stem cells, it should be fully investigated.
The study concluded:
“Our present study suggests a potential treatment strategy to reduce the putative BCSC population, and therefore enhance the effectiveness of breast cancer prevention and treatment through the use of vitamin D compounds.”
Regardless of whether DCIS or ICS really do represent a mortal threat to the health and lives of women, this study indicates that vitamin D targets the most malignant cell type found within breast cancer — the cancer stem cells — which is infinitely more selective an intervention than radiation and chemotherapy; nor does vitamin D have the profoundly damaging side effects of conventional cancer treatment.
Does this mean that women should burn their bra’s (as recommended by the feminist movement a number of years ago), and expose their breasts to the beneficial rays of the Sun? This would certainly please the males of the species, but a more private way of getting your vitamin D is with supplements. 🙂
80% of early-stage breast cancers do not progress to more concerning forms (invasive breast cancer) even after 20 years.
A 2013 study published in JAMA titled, “Over-diagnosis and Over-treatment in Cancer: An Opportunity for Improvement,” explains that the word cancer is highly misunderstood and misused.
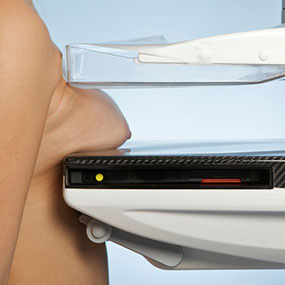
Millions of women undergo breast screening annually because their doctors tell them to do so. Not only are these women’s presumably healthy breasts being exposed to highly carcinogenic x-rays, but thousands have received a diagnosis of ‘breast cancer’ for entirely benign lesions that when left untreated would have caused no harm to them whatsoever.
The present inability of the conventional medical system to identify any clear method to determine the difference between a benign, malignant, or possibly regression-prone form of breast cancer, puts the patient at a definite risk of over-diagnosis and over-treatment, the consequences of which can be devastating to the patient and their family. The lack of individualised treatment and informed choice leads many women to undergo treatment, who may have never experienced cancer growth had they chosen to employ watchful waiting, or alternative approaches.
It has become clear that after 30 years of cancer screening with an emphasis on ‘detecting cancer early,’ the goals of such campaigns to reduce the rate of late-stage disease and decrease cancer mortality has clearly not been achieved. This would not have happened if the massive increase of diagnoses and treatment for ‘early stage’ cancer produced as a result of mammography screening over the past 25 years were actually finding ‘cancers,’ and not benign lesions that will or would not progress to malignancy.
The study explained
“Use of the term “cancer” should be reserved for describing lesions with a reasonable likelihood of lethal progression if left untreated. There are 2 opportunities for change. First, pre-malignant conditions (e.g., ductal carcinoma in situ (DCIS) or high-grade prostatic intraepithelial neoplasia) should not be labeled as cancers or tumours, nor should the word “cancer” be in the name. Second, molecular diagnostic tools that identify low-risk growths need to be adopted and validated. Another step is to reclassify such cancers as IDLE (indolent lesions of epithelial origin) conditions.”
“What has emerged has been an appreciation of the complexity of the condition called cancer. The word “cancer” often invokes the specter of a lethal process that cannot be stopped. However, cancers are diverse in nature and can follow multiple paths, not all of which progress to the spread of the disease and death, and include lazy diseases that causes no harm during the patient’s lifetime. Better biology alone can explain better outcomes.”
Unless the abnormal cell growth reaches a size at which cancer symptoms occur, it is not justifiable to treat it; nor is it appropriate to call it ‘cancer,’ as technically it is a lazy or benign lesion. Faster growing cells can contribute to symptoms over a life time, but even then, that does not mean that it will necessarily progress to cause death before natural or other causes take the patients life. In fact, premature treatment can greatly reduce the quality and length of life due to the side effects of chemotherapy, radiation, surgery, and the added stress and psychospiritual trauma of receiving a diagnosis.
Before the advent of mammography, only 3% of detected breast cancer were identified as DCIS.[1] Today, more than one-third of screen-detected early cancers are DCIS, with the unfortunate result that 33% of those diagnosed with DCIS receiving breast removal (mastectomy), 48% receiving lumpectomy and radiation treatments, 16% receiving lumpectomy, and only 3% electing to do nothing.[1] The fact that DCIS will do no harm in at least 80% of the time reveals a great burden of iatrogenic harm is being borne by women who are being coerced by an outdated treatment model that is no longer sufficiently evidence-based. However, this increased discovery rate of “cancers” can allowed massive profits to flow into the wallets of the Medical Industry at all levels. It is now apparent that the Medical Establishment is more interested in the “discovery” of benign objects within the breast and other organs, which they can label with the scary word “cancer”. Then, by playing on the fears engendered by that word the Medical Establishment can empty the wallets of the patient with impunity.
A disturbing new study published in the New England Journal of Medicine(New England Journal of Medicine, Effect of Three Decades of Screening Mammography on Breast-Cancer Incidence) is bringing mainstream attention to the possibility that mammography has caused far more harm than good in the millions of women who have employed it over the past 30 years as their primary strategy in the fight against breast cancer.[1]
Titled “Effect of Three Decades of Screening Mammography on Breast-Cancer Incidence,” researchers estimated that among women younger than 40 years of age, breast cancer was over-diagnosed, i.e. “tumors were detected on screening that would never have led to clinical symptoms,” in 1.3 million U.S. women over the past 30 years. In 2008, alone, “breast cancer was over-diagnosed in more than 70,000 women; this accounted for 31% of all breast cancers diagnosed.”
It has been estimated that 1.3 million women were falsely diagnosed with and treated for ‘breast cancer‘ in the past 30 years. These patients believe they are ‘cancer’ survivors, when in fact they are surviving the psychospiritual and physical traumas and abuses of their treatments and not their ‘disease.’ While not knowing the truth may be considered somewhat protective against further trauma associated with no longer identifying with the aggressor – i.e. the conventional medical model – and the potentially devastating realization that they have succumbed to disfigurement and poisoning from unnecessary treatments, along with co-option by cause marketing campaigns.
The journal Lancet Oncology, in fact, published a cohort study in 2011 finding that even clinically verified “invasive” cancers appear to regress with time if left untreated: (Per-Henrik Zahl, Peter C Gøtzsche, Jan Mæhlen . Natural history of breast cancers detected in the Swedish mammography screening programme: a cohort study. Lancet Oncol. 2011 Nov ;12(12):1118-24. Epub 2011 Oct 11. PMID: 21996169)
It appears that many invasive breast cancers detected by repeated mammography screening do not persist to be detected by screening at the end of 6 years, suggesting that the natural course of many of the screen-detected invasive breast cancers is to spontaneously regress.
Statin Drugs Doubles Risk of Breast Cancer
A new study published in the journal Cancer Epidemiology, Biomarkers & Prevention indicates that women who are long-term users of statin drugs have between 83-143% increased risk of breast cancer. (Jean A McDougall, Kathleen E Malone, Janet R Daling, Kara L Cushing-Haugen, Peggy L Porter, Christopher I Li. Long-term statin use and risk of ductal and lobular breast cancer among women 55-74 years of age. Cancer Epidemiol Biomarkers Prev. 2013 Jul 5. Epub 2013 Jul 5.)
Whereas recent publicity on statin drugs has focused on their potential use for cancer prevention or as anti-cancer agents, this study found exactly the opposite with current users of statins for 10 years or longer having a 1.83-fold increased risk of invasive ductal carcinoma (IDC) and a 1.97-fold increased risk of invasive lobular carcinoma (ILC) compared to women who have never used statins.
Of course, the discovery of a correlation between higher statin drug use and higher breast cancer risk does not necessarily imply causation. For instance, women who are on statins are obviously compliant with conventional blood lipid screening recommendations and therefore are more likely to be compliant with breast screening guidelines as well. Given that recent estimates show that breast screenings have resulted in over 1.3 million US women being misdiagnosed and over-treated for breast cancer in the past 30 years, simply being compliant with breast screening guidelines will result in significantly increased risk of being diagnosed with breast cancer regardless of whether the diagnosis is accurate or not.
Use of plant based diet significantly reduces risk of Breast Cancer,
In multiple studies, cancer researchers have determined that a plant-based diet and less alcohol consumption significantly reduce the risk of breast cancer.
Wasabia japonica is actually only one of hundreds of natural foods, spices and substances that have proven anti-breast cancer activity, even among drug-resistant and multi-drug resistant breast cancer cell lines.
Parsley is well known for decorating a plate, freshening your breath and getting stuck in your teeth. But did you know that it is also a cancer crusader?
Research shows this tiny green may stop the growth of breast cancer tumors associated with synthetic hormone replacement therapy.
In a study published in Cancer Prevention Research scientists exposed rats to apigenin, a common flavonoid found in parsley, other plants, fruits and nuts. The rats on apigenin developed fewer tumors and experienced significant delays in tumor formation compared to those that were not exposed to apigenin.
The finding is significant for the six to ten million women in the U.S. who use synthetic hormone replacement therapies. The authors noted that certain hormones used in synthetic HRT accelerate breast tumor development. The study exposed rats to one of the chemical progestins used in the most common HRTs prescribed in the United States — medroxyprogesterone acetate (MPA). MPA progestin is known to be the same synthetic hormone that accelerates breast tumor development.
The use of synthetic progestins as part of hormone replacement therapy has been clearly linked to an increase in breast cancer risk in postmenopausal women.
According to the researchers, when tumor cells develop in the breast in response to MPA progestin, they encourage new blood vessels to form within tumors. The blood vessels then supply needed nutrients for the tumors to grow and multiply.
But they found that apigenin blocked new blood vessel formation, thereby delaying, and sometimes stopping, the development of the tumors, and reducing the overall number of tumors.
Apigenin is most prevalent in parsley and its cousin, celery. It can also be found in:
- Chinese cabbage
- bell peppers
- apples
- cherries
- oranges
- nuts
- wine
- green tea
Parsley is the most popular herb in the world. Before it became accepted as a food, it was used medicinally and the ancient Greeks considered it sacred. In folk medicine parsley is used as a diuretic.
These new studies, together with previous studies indicate that eating a very varied diet containing a large number of different seeds and vegetables, ranging from common parsley to exotic Wasabia japonica might be a woman’s’ best defense against Breast Cancer.
Chronic Inflammation linked to Breast Cancer
Experts now believe chronic inflammation in the body may be linked to various forms of cancer as well as other major diseases such as rheumatoid arthritis, diabetes, and heart conditions. New studies continually increase our understanding of the complex inflammatory process and how it relates to breast cancer. In 2010 several pieces of the puzzle came together when researchers at Thomas Jefferson University reported they could definitively show that inflammation in the breast is key to the development and progression of breast cancer. (Liu, et al. 2010)
Green Tea reduces risk of Breast Cancer
New research from the U.S. National Institutes of Health shows that the biochemicals in green tea change a women’s estrogen metabolism, revealing at least one of its mechanisms for reducing the risk of breast cancer.
The study comes from the NIH’s National Cancer Institute, and was led by Dr. Barbara Fuhrman. The researchers tested the levels of urinary estrogens and metabolites among 181 healthy Japanese American women from California and Hawaii. Of the group, 72 of the women were postmenopausal. The remainder of the group was pre-menopausal.
The data was compiled using a combination of urinary testing along with personal interviews with each women. The woman’s intake of not only green tea, but black tea, coffee (decaffeinated or not) and soda (decaffeinated or not) was also queried and recorded and measured, and the results were adjusted with respect to caffeine consumption. Considerations such as soy consumption, body mass index, age and others were also made and adjusted.
The research found that those postmenopausal women who drank green tea daily had 20% less urinary estrone and 40% less urinary estradiol levels, when compared to those levels of women who drank green tea less than one time per week.
Final comments
From the research it would seem that there are enough natural or alternative methods for the treatment of Breast Cancer apart from the radiation, chemo or knife options. In fact, it appears that some if not most of these alternatives will be better for the patient.
From the exotic, Wasabia japonica, to the normal – Parsley and Green Tea, and just leaving well alone and staying away from X-ray equipment there appears to be a way out of the Breast Cancer problems. But, in order to achieve the result that you the Patient wants, you will need to take things into your own hands.

